What Should You Expect During Your Panniculectomy?
Posted On: April 05, 2022 Author: The Office of Dr. Stuart Linder Posted In: Breast Reduction, Plastic Surgery, Tummy Tuck
Patients requiring panniculectomy surgery show up weekly to my Beverly Hills office.
The majority of these patients have had significant weight loss, some well over 150 pounds or half their entire body weight. A significant proportion of these men and women also have had gastric bypass surgery, including Roux-en-Y, weight loss procedures and now the most popular laparoscopic banding procedure or lap band.
These patients have had significant weight loss over six months to a year and now present with massive amounts of skin hanging from the arms, chest, breasts, abdomen and thigh regions. These patients are excellent candidates for panniculectomies as they have enormous abdominal pannus. This procedure is similar to an abdominoplasty or tummy tuck; however, there is a significantly large amount of skin removed during a panniculectomy.
These patients need to first be cleared by an internal medicine specialist in order to evaluate laboratories, including Chem 20’s, CBC’s, coagulation panels as well as albumin and protein levels to evaluate their nutritional status. Subsequently, these patients are consented, all informed consents were reviewed with the patients, including risks and complications of the panniculectomy operations which can include a slightly higher risk of bleeding, hematoma, infection, skin dehiscence, wound dehiscence, fat necrosis and fat atrophy.
Panniculectomy Case Study
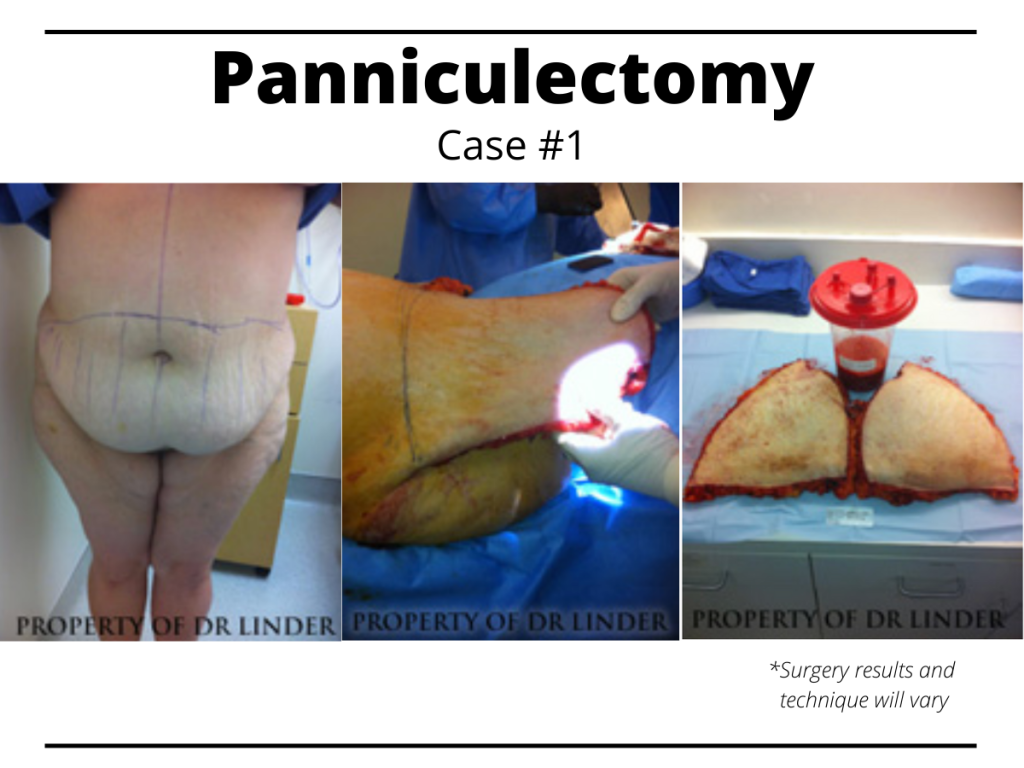
The case here (above) presents with a patient who has had a 120-pound weight loss with a massive abdominal pannus. Patient presented with stria from well above the suprapubic up to the umbilicus and above as well as intertriginous rashes, lower back pain, and mid back associated with the massive abdominal skin and adiposities.
In general, patients with a massive pannus present similar symptoms to breast reduction patients; however, instead of upper back and neck strain associated with bilateral breast hypertrophy, these patients present with lower and mid back pain as well as the significant rashes that occur, including fungal and contact dermatitis as well as staph infections.
- The operation is similar to an abdominoplasty in which an incision is made hip-to-hip and the patient placed under general anesthesia off endotracheal tube intubations, given intravenous antibiotics, the pannus is prepped and draped after local infiltration of the lower suprapubic incision site which extended to the anterior superior iliac spine or hip bilaterally.
- The entire skin was elevated all the way along the rectus and abdominal wall fascia up to the subcostal margin.
- Conservative dissection above the umbilicus was maintained in order to prevent devascularization of blood supply to the flap. The patients then have the massive amount of dermoglandular tissue resected.
- Redundant plication may or may not be performed, depending upon the degree of rectus diastasis. Often with panniculectomies the muscles are not tightened or plication of the rectus sheath is not performed.
- In any case, after removal of the massive amount of tissue as seen in the photographs, the umbilicus was repositioned into its new site and closure with three layers, including three Jackson-Pratt drains, tubes placed in for seven days.
- The patients are then placed in abdominal binders for six weeks. Tubes are removed at post-op day seven and sutures on day 17 through 21.
Panniculectomy is an excellent operation for patients who have had massive weight loss, including those with gastric bypass surgery. These are extraordinarily happy patients. The scars that are produced are well worth the removal of massive amounts of tissue that cause functional problems, including hygienic as well as severe back pain constantly.
What Goes Into a Panniculectomy?
Dr. Linder explains in the video below how he uses pre-op marking for the procedure. This patient shows a massive amount of excess skin over the abdomen and hip area after significant weight loss.
This excess will be removed during a panniculectomy procedure. During the surgery, muscles will be tightened, which may require a general surgeon to assist. The belly button will be recreated, and liposuction will be performed to help with the body contouring.
This is a functional and aesthetic operation and will help alleviate the heaviness and ease her current lower back issues.
For more information regarding panniculectomy surgery, please give us a call at (310) 275-4513 or feel free to contact us via email.