Breast Revision
in Beverly Hills, CA
Beverly Hills Breast Implant Revision Surgery
Breast implants are designed for long-term breast enhancement; however, changes in aesthetic desire or certain circumstances dictate that they must be replaced with a procedure commonly known as breast revision surgery or secondary breast augmentation.
Whether a primary augmentation has resulted in damaged implants or an unsatisfactory breast appearance, Beverly Hills plastic surgeon Dr. Stuart A. Linder can revitalize the look of your breasts with breast revision. Dr. Linder has been performing breast enhancement surgeries since 1997 and has completed over 1,000 breast revisions.
During your private consultation, Dr. Linder will evaluate your needs and desires to help determine the best technique to achieve your specific aesthetic goals. Women choose breast revision surgery to:
- Resize their implants
- Correct implant complications
- Change the placement of their implants
- Remove implants permanently
Table of Contents
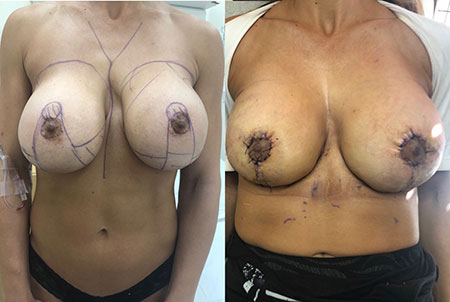
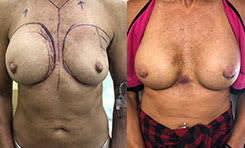
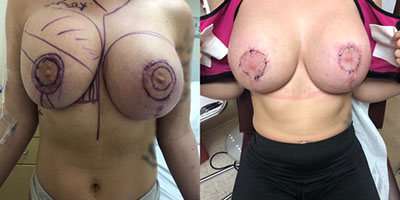
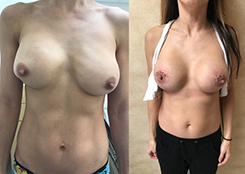
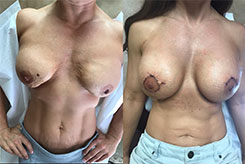
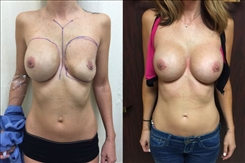
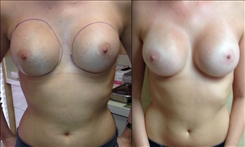
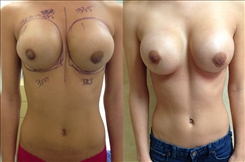
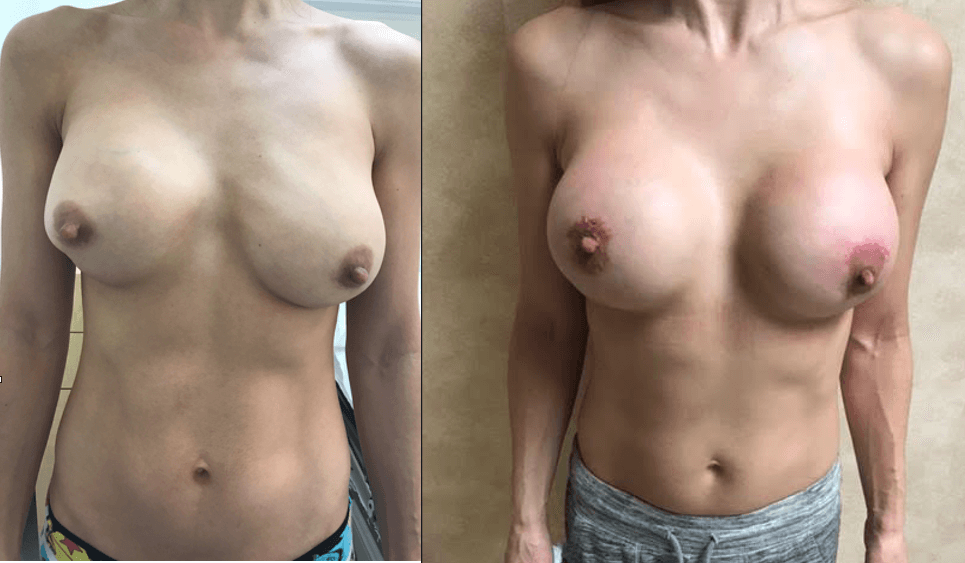
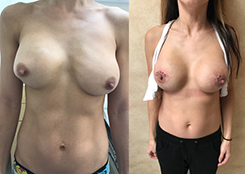
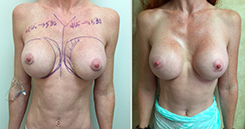
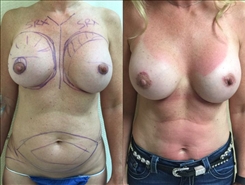
- See the Difference: Breast Revision Before & After Photos
- Real Stories: Breast Implant Revision Patient Reviews
- Breast Implant Revision Cost in Beverly Hills & Flexible Financing Options
- Why Choose Dr. Linder for Breast Revision Surgery?
- Book Your Breast Revision Consultation Today
- Why Do Patients Choose Breast Implant Revision?
- Common Breast Concerns Addressed With Revision
- Breast Revision Surgery: Ideal Candidates
- What Can I Expect From the Breast Revision Process?
- Breast Revision Surgery Steps
- After Your Revision: What Is the Normal Recovery Time for a Breast Revision?
- Breast Implant Revision Surgery Frequently Asked Questions

Real Stories: Breast Implant Revision Patient Reviews
“Dr. Linder and his team went above and beyond in revising a previous breast lift and augmentation that had left me with disappointing results from another surgeon. From the moment I walked in, Dr. Linder made me feel welcomed, hopeful, and—most importantly—safe. His specialized expertise, professionalism, and genuine care set him apart. I’m incredibly grateful for the results and the compassion I received from the entire team. If I ever need anything in the future, I wouldn’t hesitate for a second to return to Dr. Linder. Thank you so much, Dr. Linder, Adriana, and Sarai!”
– J.N. Google
“I had a revision with Dr Linder. I flew from Australia for my operation. Dr Linders’ office (Adriana) was in constant communication at all times, and it was a smooth process from start to finish with a pre-operation Zoom meeting and appointments upon arrival prior to the operation. Dr. Linder was extremely professional and listened to my needs and the size I wanted. He’s extremely precise and excellent in what he does. I have minimal scars given my revision and what was performed. They are healing very well, 3 weeks out, and I love my new size and HP shape. Sarai, the reception/office assistant, is so lovely too and very supportive and accommodating. I could not be happier with my experience and highly recommend Dr Linder and his team.”
– K. Google
Breast Implant Revision Cost in Beverly Hills & Flexible Financing Options
Many factors are considered when determining the cost of this procedure, the most significant variable being the reason for revision. Post-op complications (capsular contracture, bottoming out, rupture), a desired size change, and the type of implant being replaced must be evaluated prior to determining the cost. Additional factors include surgeon, facility, and anesthesia fees. You will receive a cost estimate for your procedure during your initial consultation with Dr. Linder.
To get a more accurate cost estimate, please contact our office for a consultation.
Why Choose Dr. Linder for Breast Revision Surgery?
Celebrity plastic surgeon Stuart A. Linder, M.D., is a board-certified plastic surgeon in Beverly Hills, California. He has over 25 years of experience performing breast revision surgery.
Dr. Linder prides himself on educating his patients throughout the process, from the consultation through the last follow-up appointment. Patients from all over the world come to Beverly Hills to see Dr. Linder and have him perform their breast revision.
Dr. Linder understands that patients will have many concerns and questions about their breast implant revision. Please contact our Beverly Hills office; our friendly staff will be happy to provide you with more information.
Book Your Breast Revision Consultation Today
Dr. Linder prides himself on educating his patients throughout the process, from the consultation through the last follow-up appointment.
Why Do Patients Choose Breast Implant Revision?
Natural Changes
Breasts tend to change over time in terms of laxity, size, and shape, regardless of whether they were previously operated on. Pregnancy, extreme weight fluctuations, and aging can all affect how the breasts look, even after augmentation. Breast revision addresses the natural changes in the breasts after augmentation and can give you a more pleasing chest appearance.
Post-op Complications
Many of the potential complications associated with breast augmentation are uncontrollable. For example, implant failure or capsular contracture may occur even in patients who received exceptional care during their initial surgery and healing process. Breast revision can correct postoperative complications, such as implant rupture, and restore a pleasing bustline.
Unsatisfactory Results
Personal preferences regarding breast aesthetics can change over time. However, sometimes the outcome of an initial breast augmentation is unsatisfying right away. When surgical results do not meet a patient’s expectations, it is appropriate to consider breast revision. Implant size, placement, and type can be modified during breast revision.
Common Breast Concerns Addressed With Revision
Capsular Contracture
Scar tissue formation is a natural response to foreign objects in the body. A capsule forms around the implant and often causes no problem. However, in some circumstances, the tissue hardens, causing pain and an irregular breast appearance. Capsular contracture is corrected through one of the following approaches:
Capsulotomy: This procedure involves expanding the capsule, softening the breast, and giving it ample room.
Capsulectomy: This procedure involves removing the implant pocket altogether, which may reduce the risk of capsular contracture recurrence.
Common Symptoms
- Painful scar tissue
- Visible distortion
- Cold and hardness to the breast
Double Bubble Breast Deformity
Double bubble breast deformity occurs when the implant is improperly placed during breast augmentation. It is quite common with the transaxillary and transumbilical approaches due to the long distance between the incision and the surgical site. To correct double bubble deformity, Dr. Linder repositions the implant and performs a breast lift to reshape the breast.
Common Symptoms
- Elevated implant
- Looseness of the lower breast skin
- Often painful scar tissue
Anatomical Breast Implant Deformity
Because anatomical breast implants are not round, any rotation in the breast pocket causes deformities that can only be fixed with breast revision. During revision, anatomical implants are often replaced with round implants, and capsulectomy may also be required to produce optimal results.
Common Symptoms
- Rotational deformity
- Postoperative implant movement
- Misshapen breast
Bottoming Out
Bottoming out occurs when implants are malpositioned during breast augmentation or when the weight of the implants weakens the lower portion of the breast. Several techniques may be implemented to repair implants that have bottomed out. It is a challenging irregularity to mend, but Dr. Linder is happy to apply his breast revision expertise to help his patients achieve the breasts they desire.
Common Symptoms
- Elevated implant
- Looseness of the lower breast skin
- Often painful scar tissue
Implant Rippling
Implant rippling and visibility can occur both above and below the muscle. Placing silicone or saline implants above the muscle in the subglandular retromammary plane does increase the risk of visibility around the medial breast, as there is no muscle coverage. However, even women who are extremely thin may develop visibility and rippling around the breast implants.
Ruptured Implants
When implants rupture, it is important to have them replaced as soon as possible to avoid excessive scarring in the breasts. If too much scar tissue has accumulated around the deflated implant, it becomes difficult to create a normal breast shape in the future.
Common Symptoms
- Painful to touch
- Visible asymmetry
- Loss of integrity to the shell
Desire for Different Implant Size
Personal preferences regarding breast size can change over the years. Many breast implant revision patients decide to exchange their implants for a different size or remove them altogether. Removal is often paired with mastopexy in cases where previous implants have caused skin laxity.
Breast Revision Surgery: Ideal Candidates
Good candidates for Beverly Hills breast implant revision are interested in removing or replacing their breast implants from an original breast augmentation surgery for health or aesthetic reasons. These women have undergone a previous breast surgery and have completely healed from that surgery. Good candidates should be in good overall health, not smoke, have realistic expectations, and have a positive outlook regarding the surgery.
Contrary to popular belief, breast implants do not need to be replaced every 10 years. If you are free from pain and happy with how your breasts look, there is likely no reason for breast revision; however, it is recommended to see a board-certified plastic surgeon if you have any concerns regarding the condition of your breast implants.
Candidates who no longer want breast implants can choose implant removal without replacement.
Contact Us
What Can I Expect From the Breast Revision Process?
Your Consultation
Dr. Linder understands that you have many questions and concerns regarding your breast revision surgery.
These questions and concerns can be addressed during your consultation. Whether you are a new patient or Dr. Linder performed your initial breast augmentation, this meeting will give you a chance to discuss your concerns and your goals for your revision.
During your consultation, Dr. Linder will:
- Examine your current implants for any noticeable complications.
- Take measurements.
- Review your medical history.
- Verify the correct techniques for your needs.
- Discuss combination procedures, such as a breast lift.
Breast Revision Surgery Steps
Preoperative
An intravenous antibiotic is given before your breast revision.
Surgery
Breast revision is performed under general anesthesia. The length of the procedure will depend on the techniques required and whether a breast lift is being performed simultaneously.
Recovery Room
Federal law requires you to remain in the recovery room for at least one hour of observation following your breast surgery.
After Surgery
You will be sent home with dressings and instructed to take oral antibiotics and pain and nausea medication for the first week. Breast revision patients should avoid heavy lifting or raising their arms above the head for at least three weeks or when cleared by Dr. Linder.
Postoperative Visit
Surgical dressings are removed. You will be recommended to wear a compression bra, such as the Dr. LinderBra™. The LinderBra™ features a double-clip zip mechanism, allowing easy placement with fresh gauze.
Day 7 Follow-Up
Dr. Linder examines your breasts for infection.
Days 8 to 14
Replace your dressings twice a day and keep your incisions clean and dry.
Day 14
All sutures will be removed.
Day 21
Dr. Linder will determine if light activities may be resumed.
Day 28
Daily activities can usually be resumed, and regular bras can be worn.

After Your Revision: What Is the Normal Recovery Time for a Breast Revision?
Most women experience a similar recovery to their initial breast augmentation. During this time, be sure to follow all of Dr. Linder’s post-op instructions and avoid any heavy lifting or strenuous activities.
What Types of Medications Will I Be Given After My Surgery?
Dr. Linder usually prescribes one of two antibiotics: Ciprofloxacin or Keflex, which is not ideal for patients allergic to penicillin. Additional pain management medications, such as Norco or Vicodin, may also be given, as well as Zofran to prevent nausea.
Will There Be Scarring After Breast Revision Surgery?
In most cases, Dr. Linder can use the same incisions as those used for your original breast augmentation. Because of this, patients tend to have minimal additional scarring after breast revision. Occasionally, additional incisions must be made or the original incisions lengthened, depending on the techniques used. Fortunately, these scars can still be hidden with bras and bathing suits.
All scars will fade over time.
What Can I Do to Help Minimize Scarring After Surgery?
Women can help minimize the visibility of their scars by following these steps:
- Avoid sun exposure on the incisions for up to one year.
- Keep the incisions clean for at least two to three weeks post-op, as this will help prevent infection.
- Keep incisions dry for at least 14 days — avoid sweating or getting the incisions wet, as this can lead to bacterial infections.
When Can I Return to Regular Activities After Breast Revision?
The length of your recovery depends greatly on the extent of correction required and the techniques used during breast revision. Usually, patients can go back to work within one week, but any strenuous activity should be avoided for at least three to four weeks.
How Long Will the Results of Breast Revision Last?
Breast revision results are considered permanent; however, the natural aging process will likely become apparent in the breasts over time. Additional complications are also possible, and patients should continue monitoring their implants.
Breast Implant Revision Surgery Frequently Asked Questions
Where Is My Surgery Performed?
Dr. Linder performs most breast revision surgeries at Summit Surgical Center in Beverly Hills, California. The surgery center is fully accredited and certified by the American Association for Accreditation of Ambulatory Surgery Facilities, Inc., and Medicare.
He also has privileges at the premier medical center, Cedars-Sinai in Los Angeles, and has been an Attending Surgeon in the Plastic and Reconstructive Surgery Division since 1997.
What Type of Anesthesia Is Used?
Breast revision at Summit Surgical Center is performed under general anesthesia and administered by a board-certified anesthesiologist. While a laryngeal mask airway is typically used, patients with a history of gastroesophageal reflux disease may opt for endotracheal intubation.
What Brands of Implants Are Used at This Facility?
Dr. Linder prefers smooth, high-profile implants by either Mentor® or Allergan™. Both are FDA-approved.
Will I Experience More Pain or Scarring Compared to My Initial Surgery?
Pain and scarring depend on the complexity of the revision surgery. Most patients find recovery comparable to their primary breast augmentation. Sometimes scarring can be minimized by using existing incisions.
What Are the Potential Risks Associated With Breast Revision Surgery?
Complications related to breast revision surgery are uncommon, but there are risks to any surgery. Some of these risks include:
- Changes in sensation
- Hematoma
- Scarring
- Unsatisfactory results
How Long Does Breast Revision Take?
Each breast revision is different depending on the cause and the techniques used. Therefore, the length of the surgery will vary. Usually, this surgery takes between 1 and 3 hours to complete. This does not include pre-op or post-op observation.
What Surgeries Are Performed in Combination?
The most common combination with breast revision is breast lift surgery. Many women choose this combination to restore a youthful, perky appearance. This combination is especially beneficial if you decide not to replace your implants or if you are replacing them to a smaller size.
Can I Change the Size, Shape, or Type of My Implants During Revision Surgery?
Yes, Dr. Linder will advise you during the consultation on the best options for size, shape, and material (e.g., silicone, saline, and profiles) based on your aesthetic goals and body type.
Will My Natural Breast Tissue Be Affected During the Revision?
In most cases, natural breast tissue remains intact. However, if a lift is combined or tissue needs reshaping, adjustments may be made to achieve optimal results.